When evaluating Medicare Advantage plans, many beneficiaries consider Aetna and Humana due to their wide range of offerings. Understanding the differences in their plans, including costs, coverage options, and additional benefits, helps in making an informed choice that aligns with healthcare needs. Both companies offer diverse plans that can vary by state, emphasizing the importance of comparing options based on individual priorities and regional availability. This guide provides insight into Aetna and Humana’s Medicare Advantage plans to equip you with the knowledge needed to navigate the selection process effectively.





Aetna vs Humana Medicare Advantage Plans
Key Highlights
- Medicare Advantage Plans provide comprehensive coverage beyond Original Medicare, including additional services from private insurers.
- Aetna and Humana offer diverse Medicare Advantage options, focusing on comprehensive coverage and flexible plan choices.
- Aetna excels in extensive network capabilities and prescription drug plans, offering robust health services and support.
- Humana emphasizes wellness and preventive care, providing fitness programs and integrative coverage options.
- The Medicare plans finder tool helps personalize comparisons, aiding beneficiaries in selecting suitable Medicare Advantage plans.
Compare plans and enroll online
Understanding Medicare Advantage Plans
Medicare Advantage Plans, a popular option among Medicare beneficiaries, offer comprehensive health coverage through private insurance companies approved by Medicare. These plans, sometimes known as Medicare Part C, encompass not only Original Medicare benefits but also additional services. Understanding the benefits of these plans can empower beneficiaries in making informed decisions about their healthcare coverage.
We’ll delve into what Medicare Advantage Plans entail and how they can impact your access to essential health services. It’s important to consider various plan features and networks when comparing options like Aetna and Humana, both pivotal players in states nationwide.
What Are Medicare Advantage Plans?
Medicare Advantage Plans, often referred to as Medicare Part C, provide an alternative to Original Medicare, offering coverage through private insurers. These plans must cover the same services as Medicare Parts A and B, including hospital stays and outpatient care. However, they differ by also covering additional benefits, such as dental, vision, and hearing services. This integration of health services makes Medicare Advantage an attractive choice for many beneficiaries looking for comprehensive coverage under a single plan, streamlining their health insurance needs.
For those considering Medicare Advantage, it’s important to understand how networks work. These plans often have network restrictions, meaning beneficiaries must use healthcare providers that are part of the plan’s network to get the lowest out-of-pocket costs. Insurance companies, like Aetna and Humana, offer various network options such as Health Maintenance Organization (HMO) and Preferred Provider Organization (PPO) plans, each with its own strengths and requirements. Understanding these network types is crucial when selecting a plan that suits personal health and financial needs.
Additionally, Medicare Advantage Plans can offer prescription drug coverage, known as Part D, which is often included in the plan’s benefits. It’s essential to look into this aspect to ensure medications are covered, potentially avoiding higher out-of-pocket pharmacy costs. As you explore Medicare Advantage options, consider using a Medicare plan finder tool to compare local offerings and tailor your choice according to coverage needs and network preferences.

Benefits of Choosing a Medicare Advantage Plan
Choosing a Medicare Advantage Plan can come with a variety of benefits that expand well beyond what Original Medicare offers. One of the distinct advantages is the inclusion of comprehensive coverage that may encompass vision, dental, and even wellness programs promoting overall health. These generous wellness benefits are designed to support a healthier lifestyle and could include access to gym memberships or routine health screenings that aren’t typically covered under standard Medicare plans.
Moreover, Medicare Advantage Plans often have a cap on out-of-pocket expenses, providing a financial safety net that protects beneficiaries from the unpredictable costs of extensive health care. This cap can be particularly beneficial to those managing chronic health conditions or those who anticipate having frequent interactions with health care providers. By capping these costs, you have better control over your health insurance and can plan financially for health-related expenses more effectively.
It’s also worth considering how Medicare Advantage Plans can offer personalized coverage through a choice of different plans, such as Aetna’s and Humana’s various options available in numerous states. Each plan with these companies offers unique coverage features and network options, allowing you to choose based on your specific health needs, whether it’s finding compatible doctors or determining which network offers the best access to specialists and hospitals. By comparing these with the use of a Medicare plan finder tool, beneficiaries can ensure they select a plan that provides optimal health insurance coverage and peace of mind.
Key Features of Aetna and Humana Medicare Plans
Aetna and Humana offer diverse Medicare Advantage options that cater to unique healthcare needs. Known for their comprehensive coverage, both companies provide an array of benefits beyond Original Medicare. Aetna is renowned for its extensive network of doctors and care options, while Humana shines with flexible plans and specialized services. Understanding these key features assists beneficiaries in selecting a plan that suits their specific requirements and preferences. In this comparison, we’ll explore Aetna’s and Humana’s offerings, covering their distinctive aspects, benefits, and network capabilities for Medicare eligible beneficiaries.
Unique Offerings in Aetna Medicare Advantage Plans
Aetna Medicare Advantage plans provide impressive benefits that extend beyond typical Medicare services. Notably, Aetna offers Medicare Advantage Prescription Drug Plans which cover a wide range of medications. This addition can be particularly helpful for beneficiaries requiring ongoing prescriptions, helping to manage out-of-pocket costs effectively.
Aetna is committed to offering a diverse range of health insurance options catering to different needs, including HMO, PPO, and Private-Fee-for-Service plans. These choices ensure a wide network of healthcare providers, allowing beneficiaries to access preferred doctors and specialists within the network, contributing to a more personalized healthcare experience.
One of the defining features of Aetna’s plans is their flexible coverage options. They offer comprehensive package deals that combine vision, dental, and hearing benefits, adding a layer of support often absent in Original Medicare. This inclusion helps beneficiaries manage their overall health better by integrating broader health services under one health plan.
Moreover, an appealing aspect of Aetna’s Medicare Advantage plans is the out-of-pocket maximum, often abbreviated as MOOP, which provides a safety net against high healthcare costs. This MOOP ensures that beneficiaries won’t face unlimited costs, offering peace of mind to those with chronic conditions or frequent healthcare needs.
The insurance Aetna provides is designed to meet diverse needs, from basic health insurance coverage to supplemental insurance benefits that offer financial protection. When comparing Aetna’s benefits with Humana’s, Aetna excels in providing extensive prescription drug plans and robust health insurance offerings. The company’s commitment to wellness programs further enhances its appeal, encouraging a healthier lifestyle through programs that include gym memberships and preventive health screenings, demonstrating Aetna’s focus on overall well-being.
Distinctive Aspects of Humana Medicare Advantage Plans
Humana Medicare Advantage plans are celebrated for their flexible and extensive coverage options tailored to diverse beneficiary needs. Humana offers various plans including Health Maintenance Organizations (HMOs) and Preferred Provider Organizations (PPOs), giving beneficiaries the freedom to choose plans that best fit their healthcare preferences. One of Humana’s standout features is its focus on wellness and preventive care, with many plans including access to fitness programs like SilverSneakers, aiming to enhance beneficiaries’ quality of life by promoting physical activity and wellness.
Humana excels in providing a broad array of benefits not just limited to routine medical care but extending to comprehensive coverage that encompasses dental, vision, and hearing services. This integrative approach ensures that beneficiaries can manage multiple aspects of their health through a single plan, simplifying their healthcare experience. Moreover, Humana offers competitive drug coverage options, ensuring that medications are more accessible and affordable for beneficiaries throughout the year.
The distinctive network capabilities offered by Humana, with their emphasis on quality and range, make it easier for beneficiaries to find care within their locality and beyond, supporting those who require specialized medical attention. Additionally, Humana offers a cap on out-of-pocket expenses, providing financial protection against unexpected healthcare costs, much like Aetna.
This feature provides beneficiaries with a level of predictability and control over their health expenses. Plans Humana provides emphasize member satisfaction, continually ranked highly for customer service, and offering convenient online tools for plan management, making accessibility and engagement with their health plans more straightforward. Lastly, Humana’s commitment to individualized care ensures that beneficiaries receive a plan that best suits their health profile and lifestyle needs.
To further explore the benefits of Humana Medicare Advantage Plans, consider these key features that enhance plan holders’ healthcare experiences:
- Fitness programs, such as SilverSneakers, promote a healthier lifestyle through regular exercise options.
- Comprehensive coverage includes essential services like dental, vision, and hearing care.
- Drug coverage with options that make medications more affordable and accessible year-round.
- Emphasis on flexible networks ensuring easy access to quality care locally and beyond.
- Cap on out-of-pocket costs offers predictable financial protection from unexpected health expenses.
- High-ranking customer service supports member satisfaction and ease of plan management.
- Convenient online tools for managing healthcare plans efficiently.
These features help personalize healthcare, making Humana Medicare Advantage a versatile and user-friendly option.
Find & Compare Plans Online
Comparing Aetna vs Humana: Coverage and Benefits
Understanding the nuances between Aetna and Humana Medicare Advantage plans can help beneficiaries choose the right coverage tailored to their needs. Both companies provide comprehensive Medicare Advantage plans, with unique offerings that distinguish them from each other. Aetna excels in robust network capabilities and prescription drug coverage, while Humana is recognized for its emphasis on wellness and preventive care. In this section, we will delve into how drug coverage and health benefits differ between these two providers, aiding beneficiaries in determining the most suitable plans for their healthcare requirements.
How Drug Coverage Differs in Aetna and Humana Plans
When evaluating Medicare Advantage plans, drug coverage is a critical factor that can significantly influence a beneficiary’s healthcare costs and plan choice. Aetna and Humana both offer extensive prescription drug plans, yet they differ in how these are integrated into their Advantage plans.
Aetna stands out with its Medicare Advantage Prescription Drug Plans, providing coverage that spans a comprehensive array of medications. These plans are particularly advantageous for those who rely heavily on prescription drugs, helping to manage copays and reduce overall pharmacy costs. Beneficiaries can access an extensive network of pharmacies, ensuring that crucial medications are readily available with minimal out-of-pocket expenses.
In contrast, Humana offers competitive drug coverage as part of its Medicare Advantage plans, but it distinguishes itself through value-added services like medication therapy management. These services help beneficiaries optimize their medication usage, potentially reducing unnecessary costs associated with medication misuse or interactions. Moreover, Humana emphasizes affordability and ease of access by offering mail-order pharmacy options, which can be highly beneficial for seniors preferring home delivery of their prescriptions.
In deciding between Aetna and Humana for drug coverage, it’s essential to review plan formularies, networks, and additional services each provides. Comparing these elements ensures that beneficiaries select a plan which not only meets their health needs but also supports financial predictability in managing their prescriptions. With both companies having extensive insurance offerings, reviewing drug coverage specifics is vital in making an informed choice.
Evaluating Health Benefits in Aetna vs Humana
Evaluating health benefits is critical when comparing Medicare Advantage plans offered by Aetna and Humana. Each company provides unique advantages that cater to diverse health needs, making a thorough review of their offerings essential.
Aetna Medicare Advantage plans are well-regarded for their comprehensive health benefits, which often include dental, vision, and hearing services as part of the package. These additional benefits can be a deciding factor for many beneficiaries seeking expansive health coverage. The inclusion of fitness programs and wellness initiatives further supports beneficiaries in maintaining a healthy lifestyle, aligning with Aetna’s holistic approach to healthcare.
Similarly, Humana’s Medicare Advantage plans are celebrated for their broad health benefits, including preventive care services designed to promote long-term wellness. Humana emphasizes physical health through initiatives like SilverSneakers, which encourages regular exercise among seniors. This focus on wellness, coupled with robust access to a wide range of healthcare providers, ensures that beneficiaries can efficiently manage their health needs. The out-of-pocket cap provided in Humana’s plans offers financial protection, which appeals to those seeking predictable healthcare expenses.
Both Aetna and Humana provide excellent Medicare Advantage plan options with distinct health benefits crafted to meet various healthcare and lifestyle requirements. When choosing between these insurers, beneficiaries should consider their specific health priorities and how the additional benefits can enhance their overall well-being. Utilizing resources like the Medicare plans finder tool can assist in comparing plan features effectively, ensuring a selection that aligns with individual health goals and financial situations.
Enrollment Considerations for Medicare Beneficiaries
Understanding enrollment considerations is essential when deciding between Aetna and Humana Medicare Advantage plans. It’s crucial to know the key enrollment periods for Medicare Advantage plans to ensure timely and proper registration. Using the Medicare plans finder tool can aid in personalized comparisons, allowing beneficiaries to choose the right health insurance that meets their unique healthcare needs. Enrollment plays a significant role in accessing the benefits of Medicare Advantage, and it’s vital to stay informed about available options in your state while considering healthcare coverage and network requirements.
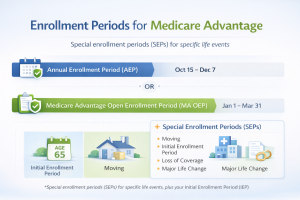
Key Enrollment Periods for Medicare Advantage Plans
Knowing the key enrollment periods for Medicare Advantage plans is pivotal for beneficiaries aiming to switch or start a new Medicare Advantage plan with companies like Aetna or Humana. The Initial Coverage Enrollment Period (ICEP) is the first opportunity for those turning 65 to enroll. This period begins three months before the month you turn 65, includes the birthday month, and ends three months after. During this time, beneficiaries can look into different plans to select coverage that aligns with their healthcare needs, whether it’s within Aetna’s robust network options or Humana’s flexible offerings.
The Annual Enrollment Period (AEP), from October 15 to December 7, is another significant window where current enrollees can review and change their Medicare plan. This period allows for the evaluation of current plans against new offerings, considering factors like coverage and network changes. Beneficiaries can pivot between Aetna and Humana, weighing differences in drug coverage and additional health benefits, ensuring they receive the most suitable plan for the coming year.
Additionally, the Medicare Advantage Open Enrollment Period, running from January 1 to March 31, offers another chance for those already enrolled in a Medicare Advantage plan to make a one-time plan change. This period is particularly useful for addressing changes in health needs or financial situations that may require different plan benefits or costs. Understanding these enrollment periods and leveraging tools like the Medicare plans finder can significantly aid beneficiaries in making informed decisions that align with their healthcare goals and financial constraints.
| Enrollment Period | Timing | Purpose | Plan Considerations |
|---|---|---|---|
| Initial Enrollment Period (IEP) | Begins 3 months before the month of the 65th birthday and ends 3 months after | To first join Medicare Parts A and B | Evaluate Part C or Part D options for additional coverage |
| General Enrollment Period (GEP) | January 1 to March 31 annually | Sign up if you missed the IEP | Consider late enrollment penalties; review available Part C/D plans |
| Annual Enrollment Period (AEP) | October 15 to December 7 annually | Modify current Medicare coverage | Compare current and new plan benefits; assess costs |
| Special Enrollment Period (SEP) | Varies based on life events | Change or enroll after qualifying events | Seek plans suited to life changes, like moving or retirement |
This table outlines essential Medicare enrollment phases and underscores the importance of personalizing healthcare selections by evaluating different plan options during these key periods. It enhances understanding by simplifying complex timelines and planning decision-making processes.
Using the Medicare Plans Finder Tool for Personalized Comparisons
The Medicare plans finder tool is an invaluable resource for beneficiaries looking to personalize their comparisons between different Medicare plans. It allows users to explore various Medicare Advantage plans offered by companies like Aetna and Humana, focusing on unique plan aspects tailored to individual needs. This tool helps in navigating through plan attributes such as coverage options, network limitations, pharmacy benefits, and the overall cost involved with each health plan.
Accessing this tool is particularly advantageous when trying to distinguish between the diverse offerings of Aetna and Humana. For instance, if you’re keen on a plan with extensive drug coverage, you might find Aetna’s offerings align better, with their Medicare Advantage Prescription Drug Plans boasting comprehensive drug lists. Alternatively, if wellness and preventive programs are more appealing, Humana’s plans, featuring initiatives like SilverSneakers, may emerge as the better fit.
The finder tool empowers beneficiaries to input their specific healthcare requirements, enabling a more precise comparison of potential Medicare Advantage plans. This personalization can encompass evaluating costs in various areas, assessing out-of-network expenses, and understanding supplemental benefits like dental and vision care that are often included in Part C plans. By using this tool to compare health insurance options, beneficiaries can ensure that they choose a plan that best matches their individual health and financial situation, thereby maximizing the benefits derived from their healthcare investment.
In conclusion, comparing Aetna and Humana Medicare Advantage plans involves evaluating key factors such as network availability, plan flexibility, additional benefits, and customer service. Both providers offer a variety of options tailored to different health needs and budgets, but personal priorities and circumstances should guide your decision.
Utilize available resources, like our Medicare plans finder tool, to explore the nuances of each plan within your locality. This careful approach ensures making an informed choice that aligns with healthcare preferences and financial plans while optimizing Medicare coverage. Remember, thorough research is the foundation of selecting the right Medicare Advantage plan.
Compare plans and enroll online
Frequently Asked Questions
What are Medicare Advantage Plans?
Medicare Advantage Plans, also known as Medicare Part C, are offered by private insurers approved by Medicare. They cover all benefits provided by Medicare Parts A and B, and often include additional services like dental and vision care.
How do Aetna and Humana Medicare Advantage Plans differ?
Aetna is known for its extensive network and prescription drug plans, providing flexibility and comprehensive health services. Humana, on the other hand, focuses on wellness and preventive care, often offering fitness programs as part of its plans.
What should be considered when choosing a Medicare Advantage Plan?
When selecting a Medicare Advantage Plan, consider costs, additional benefits like dental and vision coverage, network limitations, and prescription drug coverage. Using a Medicare plans finder tool can help compare these aspects effectively.
What is the importance of network restrictions in Medicare Advantage Plans?
Network restrictions determine which healthcare providers you can visit. Plans like HMO require using in-network providers to minimize costs, while PPO plans offer more flexibility. Understanding these restrictions ensures you choose a plan fitting your healthcare needs.
What is the Medicare plans finder tool?
The Medicare plans finder tool assists beneficiaries in comparing different Medicare Advantage Plan options based on individual healthcare needs, including coverage details, cost comparisons, and provider networks.
Have Questions?
Speak with a licensed insurance agent
1-877-436-2343
TTY users 711
Mon-Fri: 8am-9pm ET
Find & Compare Plans Online
ZRN Health & Financial Services, LLC, a Texas limited liability company

