Understanding the enrollment periods for Medicare Part C is crucial for making informed decisions about your healthcare coverage. Medicare Part C, also known as Medicare Advantage, offers beneficiaries an alternative to Original Medicare by providing additional benefits. Enrollment periods, such as the Initial Enrollment Period (IEP), Annual Enrollment Period (AEP), Special Enrollment Periods (SEPs), and Medicare Advantage Open Enrollment Period (OEP), play vital roles in determining when you can join or switch plans. Navigating these time frames ensures you make timely decisions about your healthcare needs.





Medicare Part C Enrollment Period
Key Highlights
- Medicare Part C offers an alternative to Original Medicare with additional benefits.
- Understanding enrollment periods for Medicare Advantage ensures timely healthcare decisions.
- Initial Enrollment Period allows first-time Medicare Advantage plan enrollment at 65.
- General Enrollment Period, from Jan 1 to Mar 31, caters to missed initial sign-ups.
- MedicarePartCPlans.org tool aids in comparing local Medicare Advantage plan options.
Compare plans and enroll online
Introduction to Medicare Part C Enrollment
Delving into Medicare Part C enrollment, commonly known as Medicare Advantage, offers an essential understanding for beneficiaries keen on finding the right plan. This introduction covers the basics of the enrollment periods, beginning with grasping the intricacies of Medicare Advantage Enrollment Periods. It helps you navigate your initial enrollment and ensures you make informed decisions regarding Medicare Part C, making it easier to find an Advantage plan that suits your healthcare needs. Let’s dive into how each enrollment period plays a critical role in securing comprehensive Medicare health benefits.
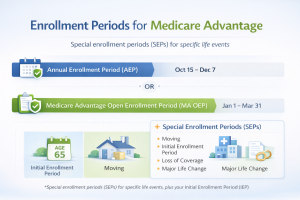
Understanding the Medicare Advantage Enrollment Period
Understanding the Medicare Advantage Enrollment Period is crucial for anyone considering joining or switching Medicare Advantage plans, also known as Medicare Part C. This enrollment period is particularly significant because it encompasses several opportunities each year for beneficiaries to select or alter their Medicare health coverage. Grasping the timelines and terms associated with these periods can drastically influence your decision-making process and overall satisfaction with your Medicare plan choices.
Firstly, we have the Initial Enrollment Period (IEP), a seven-month window that begins three months before your 65th birthday, includes your birth month, and ends three months after. The IEP is a vital phase as it’s your first opportunity to enroll in a Medicare Advantage plan if you’re eligible. Coverage starts on the first day of the month you turn 65, provided you enroll during the first three months; enrollments later during the period mean coverage may not start immediately. It’s important to use this period wisely to ensure your Medicare health strategy aligns with your current medical needs and lifestyle.
Another critical phase is the Annual Enrollment Period (AEP), running from October 15 to December 7 each year. This period allows you to switch between Medicare Advantage plans, switch from Original Medicare to a Medicare Advantage plan, or return to Original Medicare. Any changes made during the AEP will be effective from January 1 of the following year. It’s an important time to reassess your healthcare needs, possibly adjust your coverage, and review any changes proposed by your existing advantage plan’s provider.
There’s also a Special Enrollment Period (SEP), which provides flexibility beyond the usual enrollment windows. Events like moving out of your plan’s service area, losing employer coverage, or being eligible due to a federal assistance program might trigger a SEP, allowing you to select a Medicare Advantage plan outside the regular enrollment periods. Navigating these periods can be complex, so utilizing resources like the MedicarePartCPlans.org tool can prove invaluable in comparing options tailored to your specific location and health requirements.
To summarize, understanding each enrollment period’s nuances is essential. Being knowledgeable about these periods ensures that you’re well-prepared when selecting a Medicare Advantage plan. This knowledge not only helps you maximize your Medicare health coverage but also guarantees that your chosen advantage plan meets your future healthcare demands. For further assistance and a deeper exploration of Medicare enrollment periods, including how they apply to your situation, stay with us as we continue to unpack these critical elements of Medicare Part C.
Detailed Overview of Enrollment Periods
Grasping the various Medicare enrollment periods is key to effectively managing your health coverage. These periods dictate when you can join or change Medicare Advantage plans, ensuring your healthcare needs are met without unnecessary stress. The Initial Enrollment Period marks your first opportunity to enroll in Medicare, while the General Enrollment Period provides another chance for those who missed initial deadlines. Additionally, the Special Enrollment Period addresses unique situations that might affect your eligibility. Understanding these periods can significantly impact your Medicare journey, aiding in timely and informed decision-making.
Initial Enrollment Period: Your First Step into Medicare
The Initial Enrollment Period (IEP) is a crucial phase for those just becoming eligible for Medicare. This seven-month window begins three months before the month you turn 65, includes your birth month, and extends three months after. The significance of this period cannot be overstated, as it’s during these months that you can first join a Medicare plan. Enrolling during the initial enrollment ensures that your coverage starts on the first day of the month you turn 65, avoiding any unwanted gaps in health care protection. Should you miss this opportunity, you might face an enrollment penalty, impacting future premiums and possibly delaying your coverage start date.
In addition to those turning 65, the IEP applies to others eligible for Medicare due to certain disabilities or specific health conditions, such as End-Stage Renal Disease. Understanding when you’re eligible to join or whether you need additional forms to complete your enrollment is essential. Many find navigating the Medicare program’s details complex, but resources like MedicarePartCPlans.org simplify this by providing clear, unbiased information on plan options available in your area.
As you approach the Initial Enrollment Period, it’s advisable to consider your long-term health care needs. Evaluate whether a Medicare Advantage plan (Part C) might better serve you than Original Medicare. These advantage plans often include additional benefits, such as vision, dental, or hearing, and they cap out-of-pocket expenses. However, it’s vital to examine each plan’s network of doctors and facilities, ensuring they align with your current providers. Should questions arise regarding your specific situation, don’t hesitate to consult with trusted resources.
Failing to enroll during this period when first eligible often results in higher costs down the line. Penalties for late enrollment apply to Part B and potentially Part D if you delay joining without credible coverage. These penalties can accumulate over time, reflecting the importance of timely enrollment. Proactively engage with resources and tools available to you, such as online Medicare advantage plan finders, to ensure you make informed decisions about your health coverage.
Find & Compare Plans Online
General Enrollment and Its Significance for Medicare Beneficiaries
The General Enrollment Period (GEP) is another vital segment of Medicare’s enrollment periods, providing opportunities for those who missed the Initial Enrollment Period to sign up for Part B (and potentially Part A). Held annually from January 1 to March 31, the general enrollment allows individuals to enroll in Medicare coverage for the first time or make adjustments if necessary. Coverage for those who enroll during this period begins on July 1, emphasizing the importance of timely decision-making to avoid extended periods without necessary health insurance.
Many beneficiaries find themselves relying on the General Enrollment Period due to unawareness or life circumstances that delayed their initial sign-up. It’s crucial to understand that enrolling during this period can introduce an enrollment penalty for late Part B coverage, adding to your monthly premiums for as long as you have Part B. Understanding the implications of missing early enrollment periods and planning accordingly can mitigate these costs.
During the GEP, evaluating whether to join a Medicare Advantage plan is equally important as enrolling in Original Medicare. This decision can impact your access to additional health benefits and out-of-pocket costs under Medicare plans. Medicare Advantage plans often offer a bundled approach to coverage, integrating Medicare Part A, Part B, and sometimes Part D, along with extra health benefits like fitness programs, medical transportation, or telehealth services. Part C may include prescription coverage. As you consider joining or switching plans, reflecting on your past medical expenses and expected future needs can help guide your choice.
Plan exploration tools, such as those offered by MedicarePartCPlans.org, are beneficial in this regard. They allow you to compare Medicare Advantage options efficiently, considering both national and local plan variations. Medicare’s General Enrollment provides an imperative opportunity to reassess health needs annually. Whether seeking to join for the first time or explore Medicare’s additional benefits, this period ensures beneficiaries remain informed and prepared.
While General Enrollment provides a second chance to join Medicare or adjust coverage, proactive engagement during the Initial Enrollment Period or Special Enrollment instances remains ideal. Each period caters to different needs and opportunities, emphasizing foresight and understanding in managing Medicare choices efficiently.
| Enrollment Period | Eligibility Criteria | Key Actions |
|---|---|---|
| Initial Enrollment Period (IEP) | Begins 3 months before you turn 65, includes the month you turn 65, and ends 3 months after | Sign up for Medicare Part A and Part B |
| General Enrollment Period (GEP) | For those who missed, the IEP occurs from January 1 to March 31 annually | Enroll in Medicare Part A and/or Part B with coverage starting July 1 |
| Special Enrollment Period (SEP) | Triggered by specific life events, such as losing employer coverage | Allows enrollment outside standard periods without late penalties |
| Annual Enrollment Period (AEP) | October 15 to December 7 each year | Make changes to the Medicare Advantage or the Prescription Drug plan |
This table highlights how Medicare enrollment periods play a critical role in effective health coverage management.
Special Enrollment Period: Addressing Unique Circumstances
The Special Enrollment Period (SEP) introduces flexibility in Medicare’s usually rigid enrollment framework, accommodating life changes that might affect your eligibility or needs. Unlike fixed windows such as the Initial or General Enrollment Periods, SEPs are triggered by qualifying life events. Events prompting a SEP can include moving out of your current plan’s service area, losing other health coverage, or changes in eligibility due to federal assistance programs.
For eligible individuals, the Special Enrollment Period offers invaluable opportunities to join or switch plans without the typically associated penalties. Importantly, many find SEPs essential when facing unexpected life events. For example, if you move to a new location with different available Medicare Advantage plans, a SEP allows you to transition your healthcare seamlessly to better suit your new circumstances.
Additionally, understanding when a SEP might apply helps in avoiding costly gaps in coverage. SEP eligibility frequently arises when health coverage changes, such as losing group health insurance from a former employer. During such transitions, it’s critical to act quickly to enroll in a Medicare Advantage plan that accommodates your health and financial needs. The MedicarePartCPlans.org resources can aid significantly during this period, simplifying plan comparisons and choices based on your new location’s offerings and requirements.
Moreover, SEPs underscore the importance of being informed about Medicare’s broader enrollment framework. For existing beneficiaries, a change in income can occasionally permit an adjustment in Medicare plan selections, particularly if you become eligible for additional financial assistance programs or Medicaid. Leveraging these special periods ensures that your Medicare coverage remains both relevant and cost-effective.
The flexibility of a SEP helps tailor your Medicare experience to your unique life journey, providing peace of mind when confronted with personal and financial changes. As each SEP comes with specific timeframes and eligibility rules, staying alert to how these factors align with your circumstances is crucial. By understanding and appropriately acting during SEPs, beneficiaries can maintain optimal coverage without unnecessary delays or financial penalties. Always consider using reliable venues like MedicarePartCPlans.org for guidance and updated information tailored to your specific situation.
Exploring Medicare Plan Options by Location
Evaluating Medicare plan options based on your location is essential for ensuring that your healthcare needs are met efficiently. The types of plans available, including Medicare Advantage, can vary significantly from one area to another, making location a critical factor in your decision-making process. Through the use of tools such as MedicarePartCPlans.org’s comparison tool, beneficiaries can access a wide range of information about the plans available, tailored to their location. This tool simplifies the process of finding and comparing plans, allowing beneficiaries to make informed choices with confidence about their healthcare coverage.

Using the MedicarePartCPlans.org Tool to Compare Plans
Navigating the intricate landscape of Medicare plans can be daunting, especially when considering location-specific options like Medicare Advantage plans. MedicarePartCPlans.org provides an invaluable tool that eases this process by allowing users to find, compare, and evaluate various plans based on their specific geographic area. This tool’s core function is to align available plans with the individual needs of beneficiaries, considering the variations in plan offerings that often occur due to regional factors.
For example, some plans might include additional benefits like dental or vision tailored to local provider partnerships, crucial details that can directly affect out-of-pocket costs and coverage satisfaction.
Using the tool is straightforward, starting with entering your specific location details. This ensures the results are precise, giving you access only to plans pertinent to your area. With location being such a pivotal factor in determining plan types and availability, beneficiaries can zero in on options that are realistically accessible and relevant, reducing the risk of enrolling in a plan that does not operate in their region.
Once your location is set, the comparison tool allows insight into different plan structures, premium variations, and the extent of network providers available. Coverage options can vary; some plans might offer comprehensive Medicare health benefits, inclusive of services not covered under Original Medicare. Assessing these through the comparison tool enables you to visualize potential savings or additional costs associated with each plan.
For those already enrolled in Medicare but looking to switch to a different Medicare Advantage plan during an enrollment period, the tool becomes a valuable resource for evaluating current satisfaction with network services and coverage adequacy.
Moreover, the tool enhances understanding by offering an easy-to-negotiate interface that presents plan details side-by-side. This transparency is designed to empower users, providing them with the necessary details such as plan ratings, provider networks, and customer service quality. Together, these metrics are essential when considering a switch or initial enrollment in a Medicare Advantage plan, ultimately aiding in making education-driven decisions tailored to individual health needs and preferences.
For caregivers assisting family members in finding appropriate Medicare health coverage, the MedicarePartCPlans.org tool simplifies what can be a complex process. By efficiently narrowing options based on location-specific offerings, this tool minimizes the stress associated with understanding Medicare’s layers. Additionally, since the landscape of available advantage plans can shift annually due to changes in regional healthcare contracts or Medicare policy adjustments, the tool is continually updated to reflect such changes, solidifying its role as a reliable source of current plan information.
Therefore, engaging in regular comparisons using dedicated tools allows beneficiaries to stay informed about the evolving landscape of Medicare Advantage plans, ensuring their healthcare coverage remains both relevant and cost-effective. With technology playing an increasingly valuable role in healthcare decision-making, leveraging resources like the MedicarePartCPlans.org comparison tool is vital for beneficiaries eager to optimize their Medicare Advantage plan choices based on their specific location’s offerings.
To further enhance your understanding of how to effectively utilize the MedicarePartCPlans.org tool, consider these practical tips:
- Start by gathering personal and geographic details for a more tailored plan search.
- Familiarize yourself with key insurance terms to navigate plan features confidently.
- Utilize the tool regularly to keep updated on plan changes and new offerings.
- Compare not just costs, but also additional benefits offered by different plans.
- Assess network provider accessibility to ensure your preferred doctors are included.
- Read user reviews to gain insights into plan performance and customer service.
- Consult with healthcare advisors when needed to complement the tool’s guidance.
Each of these tips will aid in your journey to select a Medicare Advantage plan that meets your needs seamlessly.
Understanding Medicare Part C enrollment periods is crucial for making informed choices about your healthcare coverage. Knowing when and how you can enroll or make changes to your plan helps ensure you have access to the benefits that align with your needs. For assistance in navigating your Medicare Part C options, consider using resources like our Medicare plans finder tool to compare various plans based on your location and specific coverage needs. With the right understanding and resources, you can confidently choose the Medicare Advantage plan that best suits your requirements.
Compare plans and enroll online
Frequently Asked Questions
What is Medicare Part C?
Medicare Part C, also known as Medicare Advantage, offers beneficiaries an alternative to Original Medicare by providing additional benefits. It includes coverage for services covered under Part A and Part B, often with additional benefits like vision and dental.
When can I enroll in Medicare Part C?
You can enroll during several enrollment periods: Initial Enrollment Period (IEP), Annual Enrollment Period (AEP), Special Enrollment Periods (SEPs), and Medicare Advantage Open Enrollment Period (OEP). Each period has specific eligibility criteria and timing.
How does the Initial Enrollment Period (IEP) work?
The IEP is a seven-month window starting three months before you turn 65, including your birth month, and ending three months after. During this time, you can enroll in a Medicare Advantage plan if you’re eligible, ensuring you have coverage when you turn 65.
What is the Annual Enrollment Period (AEP)?
The AEP runs from October 15 to December 7 each year. It’s a time when you can switch Medicare Advantage plans, switch from Original Medicare to Medicare Advantage, or return to Original Medicare. Changes take effect on January 1 the following year.
What is a Special Enrollment Period (SEP)?
SEPs allow you to enroll or switch plans outside the usual enrollment periods due to life events like moving out of your plan’s service area, losing employer coverage, or becoming eligible for a federal assistance program. Eligibility and timing vary based on the event.
Have Questions?
Speak with a licensed insurance agent
1-877-436-2343
TTY users 711
Mon-Fri: 8am-9pm ET
Find & Compare Plans Online
ZRN Health & Financial Services, LLC, a Texas limited liability company

