Discover comprehensive healthcare coverage options with Medicare Part C Plans in Ohio 2027. Known as Medicare Advantage, these plans combine Original Medicare Parts A and B, offering additional benefits such as dental, vision, and prescription drug coverage. Navigating the wide range of options can be challenging, but understanding your specific health needs and budget is key. Our independent educational resources are designed to simplify your search and help you compare plans available in Ohio. Explore the advantages of Medicare Part C and find a plan that aligns with your healthcare requirements and lifestyle preferences.





Best Medicare Part C Plans Ohio 2027
Key Highlights
- Medicare Advantage plans in Ohio offer additional benefits like dental and vision beyond Original Medicare.
- Choosing between HMO and PPO plans affects network flexibility and out-of-pocket costs for enrollees.
- Seniors can benefit from comprehensive coverage, including prescription drugs and wellness programs.
- Important enrollment periods include AEP from October 15 to December 7, and MA OEP from January 1 to March 31.
- Utilize the Medicare plans finder tool to compare local Medicare Advantage options in Ohio.
Understanding Medicare Advantage Plans in Ohio
Exploring Medicare Advantage plans in Ohio reveals essential nuances for beneficiaries seeking comprehensive coverage. These plans, also known as Medicare Part C, offer an alternative to Original Medicare by combining health insurance options with additional benefits. As Medicare Advantage plans vary in terms of network arrangements, costs, and coverage, understanding these elements is crucial for making informed decisions. This section delves into factors such as plan selection criteria and the differences between HMO and PPO offerings, providing Ohio residents with the insight needed to choose the right plan for their healthcare needs.
What to Consider When Choosing a Plan
When selecting a Medicare Advantage plan, also known as Part C, there’s much to ponder to ensure it aligns with your health coverage needs. The diverse options available in Ohio make it critical to evaluate several key factors. First, consider the network size associated with different plans. Medicare Advantage plans typically require you to use a network of doctors, hospitals, and other healthcare providers. This network can significantly impact your out-of-pocket costs, particularly if you prefer a specific provider who may not be in-network. Therefore, it’s vital to scrutinize the network details of any potential advantage plans you consider.
Another key consideration is the cost structure of the Medicare Advantage plans. This encompasses not just monthly premiums but out-of-pocket expenses such as copayments, coinsurance, and deductibles. While some plans may offer lower premiums, they might have higher cost-sharing requirements, which can affect your overall healthcare expenses. Be attentive to how each plan structures these costs and how they align with your healthcare budget and needs.
Medicare Advantage plans often include benefits that go beyond traditional Medicare, such as dental, vision, and hearing coverage. Assess which additional benefits are pertinent to you and whether these enrichments justify any potential cost differences. This is particularly true for dental coverage, which isn’t included under Original Medicare.
Each plan type, whether it’s an HMO or PPO, comes with specific enrollment rules and resource availability. Be sure you understand these to avoid coverage gaps. Enrollment periods are crucial too; they’re the windows when you can sign up or make changes to your coverage. Missing these could mean waiting until the next period, resulting in uncovered needs.
Research and possibly use a Medicare plans finder tool can facilitate the process. Ultimately, taking the time to understand these factors will aid in selecting a plan that’s not only comprehensive but tailored to your specific healthcare preferences and financial considerations.

Differences Between HMO and PPO Options
When diving into the realm of Medicare Advantage plans, understanding the differences between Health Maintenance Organization (HMO) and Preferred Provider Organization (PPO) options is essential. Both plan types provide coverage as part of the Medicare Advantage program, but they operate under different rules, particularly regarding network structure and flexibility.
HMOs are known for their cost-effectiveness, making them appealing if budget is a significant factor. However, these plans generally require members to choose a primary care physician who coordinates their care and provides referrals to see specialists. This gatekeeper model helps control healthcare costs but might not offer the flexibility some beneficiaries desire, especially if they wish to see out-of-network specialists without a referral. Moreover, HMO plans typically restrict coverage for non-emergency services outside their network, potentially limiting provider choice.
In contrast, PPO plans offer greater flexibility by allowing beneficiaries to seek services from both in-network and out-of-network providers. While using in-network services usually results in lower out-of-pocket costs, the option to go out-of-network provides added flexibility, which can be particularly beneficial in areas with limited provider choices.
It’s crucial to assess your own healthcare needs and provider preferences when considering these options. If you value lower costs and are comfortable working within a network with a fixed healthcare team, an HMO might be suitable. Conversely, if you prefer having the option to visit specialists without referrals and flexibility in choosing healthcare providers, a PPO may align better with your needs.
The decision between HMO and PPO Medicare Advantage plans involves weighing the benefits of cost savings against the convenience and flexibility of provider access. Knowing how each plan type fits into the broader context of your health insurance strategy will inform better alignment with your healthcare goals. Understanding these differences ensures that you make an informed choice, maximizing your Medicare Advantage benefits in Ohio.
Here’s a detailed look at how each factor might impact your choice between HMO and PPO Medicare Advantage plans in Ohio:
- Specialist Consultations: If you frequently need specialist consultations and prefer not to get a referral, a PPO plan might suit you better, as it generally allows more direct access to specialists without referrals, unlike HMOs, which typically require a primary care physician referral.
- Travel and Provider Access: For those who travel often or live between states, a PPO plan offers more flexibility with out-of-network providers, making it easier to get care in different locations, whereas HMO plans may restrict you to a local network.
- Healthcare Expenses: It’s vital to compare current healthcare costs with the premiums, deductibles, and co-payments of each plan. HMOs often have lower out-of-pocket costs but less flexibility, while PPOs might offer savings through broader provider options.
- Consistent Healthcare Team vs. Broad Network: An HMO often means staying within a specific network, fostering familiarity with a consistent team. In contrast, a PPO provides access to a wider range of providers, albeit often at higher costs.
- Predictability vs. Flexibility in Costs: If you value stable, predictable costs, an HMO might be preferable. If you’re willing to pay more for the flexibility of seeing out-of-network providers, a PPO might be more appealing.
- Provider Selection vs. Care Coordination: Consider if the freedom to select any provider is more important than the structured care coordination an HMO can offer, where your care team communicates seamlessly.
- Additional Benefits: Some plans may offer extra perks like wellness programs, gym memberships, or vision/dental coverage. Assess how these benefits align with your lifestyle and whether they enhance the value of the plan for you.
Evaluating these nuances will guide you in choosing a plan that best suits your healthcare needs and preferences, ensuring you receive the desired balance of cost, access, and care quality.
The Benefits of Medicare Advantage for Seniors
Medicare Advantage plans offer a host of benefits that can significantly enhance the healthcare experience for seniors. These plans, also known as Medicare Part C, provide more than just the basics of Medicare; they bundle additional services like vision, dental, and hearing coverage, which are not included in Original Medicare. For Ohio seniors looking to broaden their healthcare options, Medicare Advantage plans offer a comprehensive package that can simplify managing medical needs. By understanding the coverage, costs, and additional benefits, seniors in Ohio can make informed choices that cater to their health and financial needs.
| Coverage Details | Wellness & Preventive Services | Cost Considerations | Geographic Variance | Out-of-Pocket Protection |
|---|---|---|---|---|
| Includes vision, dental, and hearing benefits. | Offers gym memberships and telehealth resources. | Details on premiums, copayments, and deductibles. | Plan availability and pricing vary by location. | Annual out-of-pocket maximums cap expenses. |
This table illustrates the multifaceted nature of Medicare Advantage plans, emphasizing the integrated care and financial considerations beneficial for Ohio seniors.
Comprehensive Coverage Explained
Diving into comprehensive coverage under Medicare Advantage plans reveals why these options are so appealing to seniors. One of the main draws is the ability to receive coverage for services beyond what Original Medicare offers, including vision, dental, and hearing care, which are essential as health needs evolve in later years. This additional coverage can significantly influence quality of life, as it allows seniors to take a proactive approach in managing and maintaining their health.
Many Medicare Advantage plans in Ohio also include prescription drug coverage, which consolidates your healthcare needs into a single plan and can simplify the management of medication needs.
Beyond traditional medical and prescription drug coverage, the benefits of Medicare Advantage plans extend to wellness programs and preventive services. Plans may offer benefits like gym memberships or discounts on health-related activities, encouraging a healthier lifestyle. This integration of health-promoting services aligns well with the goal of comprehensive coverage, ensuring all-encompassing care that addresses both immediate health issues and preventive strategies.
Understanding the network structure of Medicare Advantage plans is also pivotal for maximizing comprehensive coverage. These plans often require enrollees to select primary care providers and encourage the use of in-network specialists and hospitals. While this might seem restrictive compared to Original Medicare, it allows for coordinated care which can reduce medical costs and improve health outcomes through streamlined communication amongst healthcare providers.
Additionally, plans can include resources like telehealth services, which offer the convenience of receiving medical advice and consultations from the comfort of home. This can be especially beneficial in reducing exposure to potential health risks and ensuring timely care, particularly in managing chronic conditions. When seniors evaluate these comprehensive coverage options, weighing the advantages of integrated care and additional benefits can be crucial in selecting a plan that best meets their personal health requirements and lifestyle goals.
Comparing Cost and Out-of-Pocket Expenses
Costs associated with Medicare Advantage plans can vary widely, making it critical to compare pricing structures to find the best fit. Initial considerations often start with the premiums, which can be surprisingly low for many plans, yet this is just one piece of the cost puzzle. Seniors need to consider other out-of-pocket expenses like copayments, coinsurance, and deductibles, which vary from plan to plan. Understanding these costs is fundamental to ensuring the affordability of comprehensive health coverage under Medicare Advantage.
When considering these plans, seniors need to assess how these out-of-pocket expenses might impact their healthcare budget. Some plans with low premiums might have higher copayments for doctor visits or hospital stays, while others might offer more predictable costs with higher premiums but lower copayments and coinsurance. This balance can be particularly important for those on a fixed income, where predicting monthly expenses helps in managing overall finances more effectively.
Location can also play a significant role in costs across states like Pennsylvania, and plan availability and pricing often vary across Ohio. It’s wise for beneficiaries to use tools, such as the Medicare plans finder tool, to compare local plan options that align with their healthcare needs and financial limitations. Evaluating factors like network size and accessibility alongside cost factors can give a complete picture of the practicalities of each plan.
A crucial part of cost comparison is understanding the annual out-of-pocket maximum. This is often a protection feature of Medicare Advantage plans, ensuring seniors won’t spend beyond a capped amount for covered services each year, offering peace of mind against excessive medical expenses. By comparing these limits alongside other out-of-pocket costs, seniors can find the right Medicare Advantage plan tailored to their specific needs and financial constraints. This careful consideration ensures that the benefits of Medicare Advantage truly align with and support their health and wellness goals without causing financial strain.
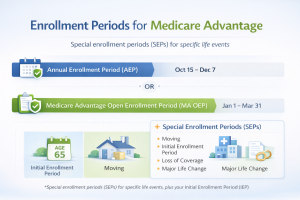
Enrollment Periods for Medicare Part C Plans
Understanding the enrollment periods for Medicare Part C plans is essential for Ohio residents considering Medicare Advantage plans. These periods define when you can initially sign up or make changes to your coverage. This section outlines the important dates and enrollment opportunities critical for planning your healthcare to ensure you have the right coverage when you need it. Knowing these timeframes helps prevent lapses in coverage, maximizing your Medicare Part C benefits.
Important Dates for Ohio Residents
Navigating the maze of Medicare Part C enrollment periods is crucial for residents of Ohio. The Annual Enrollment Period (AEP) is one of the most significant times, occurring from October 15 to December 7 each year. During the AEP, you can switch, drop, or join a Medicare Part C plan, making it an essential period for planning your healthcare strategy. Ohio residents should mark these dates on their calendars, as it ensures they can make changes to their coverage without any penalties or delays. Missing this window could mean waiting another year to adjust your plan, potentially impacting your medical coverage and out-of-pocket expenses.
For those new to Medicare, the Initial Enrollment Period (IEP) is a critical step in starting your Medicare journey. This seven-month period begins three months before your 65th birthday, includes the birth month, and extends three months afterward. Understanding when to enroll can help you avoid any gaps or delays in coverage. Ohioans turning 65 should use this time wisely to assess their healthcare needs and explore different Medicare Advantage options. Utilizing resources like the Medicare plans finder can simplify the comparison process, helping uncover the most suitable plan for your medical and financial situation.
Another period to consider is the Medicare Advantage Open Enrollment Period, which runs from January 1 to March 31. Within this window, individuals who are already enrolled in a Medicare Advantage plan have the opportunity to make changes. Whether it’s switching plans or returning to Original Medicare, this timeframe provides a valuable opportunity for residents of Ohio to optimize their coverage if their current plan no longer meets their needs. It reflects the flexibility inherent in Medicare Advantage plans, catering to evolving medical and financial circumstances.
For those dealing with specific life changes like moving out of their plan’s service area like to another state such as Illinois, or experiencing other eligible circumstances, a Special Enrollment Period (SEP) might open up. This period is invaluable for ensuring continuous coverage without facing penalties due to unforeseen personal changes. Understanding the nuances of SEPs empowers Ohio residents to maintain consistent coverage, protecting against potential disruptions in their healthcare services.
Planning effectively for these enrollment periods involves staying informed about the important dates and understanding how each period impacts your Medicare plan choices. Whether it’s tapping into the comprehensive benefits or finding a network that aligns with your medical needs, keeping on top of the enrollment schedule is crucial. Using resources and educational tools provided by services like MedicarePartCPlans.org can guide this exploration, ensuring you maximize your Medicare Advantage benefits effectively.
As you explore Medicare Advantage (Part C) plans in Ohio, it’s essential to carefully consider your individual healthcare needs and financial situation. With a wide range of options available, you can find plans varying by coverage, provider networks, and added benefits. Take advantage of resources like the free Medicare plans finder tool on MedicarePartCPlans.org to compare offerings specific to your location. Whether you’re new to Medicare or reviewing your annual choices, being informed will help you make empowered decisions about your healthcare. Thank you for visiting MedicarePartCPlans.org, your trusted resource for Medicare education.
Frequently Asked Questions
What are Medicare Advantage plans, and how do they differ from Original Medicare?
Medicare Advantage plans, also known as Medicare Part C, combine Original Medicare Parts A and B and usually offer additional benefits like dental, vision, and prescription drug coverage. These plans are an alternative to Original Medicare and are provided by private insurance companies. They often have different network arrangements and cost structures.
What are the key differences between HMO and PPO Medicare Advantage plans?
HMO (Health Maintenance Organization) plans generally require members to choose a primary care physician and get referrals for specialists, limiting out-of-network services. PPO (Preferred Provider Organization) plans offer more flexibility, allowing services from both in-network and out-of-network providers but typically at a higher cost for out-of-network services.
When are the enrollment periods for Medicare Advantage plans?
The Annual Enrollment Period (AEP) runs from October 15 to December 7 each year, allowing changes in coverage. The Medicare Advantage Open Enrollment Period (MA OEP) is from January 1 to March 31, letting enrollees make further alterations. Initial Enrollment Periods and Special Enrollment Periods also apply in certain conditions.
How can beneficiaries in Ohio compare different Medicare Advantage plans?
Beneficiaries can compare plans using resources like the Medicare plans finder tool on MedicarePartCPlans.org. This tool helps in evaluating local plan options based on coverage, costs, and other personal healthcare needs.
What additional benefits do Medicare Advantage plans usually include?
Medicare Advantage plans often include benefits not offered by Original Medicare, such as dental, vision, hearing coverage, and sometimes wellness programs or gym memberships. Prescription drug coverage is also frequently included, consolidating healthcare needs into one plan.
ZRN Health & Financial Services, LLC, a Texas limited liability company

