Understanding who regulates Medicare Advantage Plans is crucial for beneficiaries exploring their healthcare options. Medicare Advantage, also known as Part C, operates under the guidance of the Centers for Medicare & Medicaid Services (CMS), ensuring these plans meet federal standards. This page will provide insights into CMS statutes and an overview of the diverse plans available, helping you comprehend the regulatory framework that shapes these offerings. Whether you’re new to Medicare or reevaluating your current plan, this information is designed to clarify how Medicare Advantage plans are structured and controlled.





Who Regulates Medicare Advantage Plans?
Key Highlights
- Medicare Advantage plans offer comprehensive coverage through private insurers, approved by Medicare.
- CMS regulates Medicare Advantage, ensuring benefits meet federal standards and protect enrollees.
- Medicare Advantage plans often include dental, vision, and prescription drug coverage, unlike traditional Medicare.
- Location-based comparison tools help beneficiaries select suitable Medicare Advantage plans tailored to local networks.
- Special Enrollment Periods offer flexibility to adjust Medicare plans during life changes without penalties.
Compare plans and enroll online
Understanding Medicare Advantage Plans
Medicare Advantage plans, also known as Medicare Part C, offer an alternative to traditional Medicare by providing comprehensive coverage through private insurance companies. This section will explore how Medicare Advantage varies from traditional Medicare and highlight some of the common benefits these plans offer. With this knowledge, you’ll be better equipped to understand if a Medicare Advantage plan meets your health coverage needs. Tailoring the selection of plans to individual needs and understanding the differences can help maximize the benefits you receive.
How Medicare Advantage Differs from Traditional Medicare
Medicare Advantage plans differ significantly from traditional Medicare in a number of ways, offering a comprehensive alternative for those seeking additional coverage through private insurers. One of the main differences lies in how these plans are offered and managed. While traditional Medicare provides Part A and Part B directly, Medicare Advantage plans are offered by private insurance companies approved by Medicare. They bundle Parts A and B, often including Part D for prescription drug coverage. This integration provides a streamlined and often more cost-effective approach to coverage for many beneficiaries.
Another distinct difference is how healthcare networks function under Medicare Advantage. Unlike traditional Medicare, which allows beneficiaries to see any doctor who accepts Medicare, Medicare Advantage plans typically operate through managed care models such as HMOs (Health Maintenance Organizations) or PPOs (Preferred Provider Organizations).
These networks may require members to use healthcare providers within a specific network, ensuring coordinated care and often reducing out-of-pocket expenses. This model can be advantageous for those who prefer structured care plans, but it might limit the flexibility some beneficiaries appreciate under traditional Medicare.
One critical factor for beneficiaries considering Medicare Advantage is understanding the cost structure involved. While traditional Medicare has a standardized premium, deductible, and coinsurance structure, costs under Medicare Advantage can vary widely depending on the plan selected. Some plans may offer additional benefits such as dental, vision, or wellness programs, which are not typically covered by traditional Medicare, providing greater flexibility and appeal to a diverse range of health care needs.
It’s important to carefully review each plan’s specifics because the cost-sharing responsibilities, including premiums and copayments, may differ significantly between plans and from traditional Medicare.
Risk adjustment is another element where Medicare Advantage and traditional Medicare diverge. The Centers for Medicare & Medicaid Services (CMS) use a risk adjustment model to determine reimbursement levels to Medicare Advantage plans. This methodology adjusts payments based on the health condition and demographic characteristics of enrollees, ensuring that plans are adequately compensated for covering sicker or medically complex populations. Traditional Medicare, on the other hand, uses a fee-for-service payment model that pays providers directly for the services rendered.
Understanding these differences is crucial for Medicare beneficiaries to make an informed decision about their healthcare. With Medicare Advantage, individuals have the option to receive additional services and more integrated care management, potentially improving overall health outcomes. However, it’s important to weigh these benefits against the network restrictions and variable costs compared to traditional Medicare. Utilizing resources like those available on MedicarePartCPlans.org can assist beneficiaries in navigating these choices effectively.

Common Benefits Offered by Medicare Advantage Plans
Medicare Advantage plans are well-regarded for their range of additional benefits, often surpassing what traditional Medicare offers. One of the primary attractions is the inclusion of routine dental, vision, and hearing care, services not typically covered under traditional Medicare. For many beneficiaries, these services are crucial for maintaining overall health, especially as age-related issues in these areas can frequently arise. Medicare Advantage makes these benefits accessible, thus preventing higher out-of-pocket expenses that might otherwise occur.
Moreover, many Medicare Advantage plans provide prescription drug coverage, simplifying the enrollment process by combining it with the primary health insurance coverage. This integration often results in lower overall drug costs and a cohesive prescription management system. Some plans may also offer fitness benefits, like memberships to gyms or discounts to wellness programs, promoting physical activity and well-being which can contribute significantly to better long-term health.
Furthermore, some plans encompass transportation services to and from medical appointments, a significant benefit for those with mobility challenges or limited access to reliable transportation. Accessing healthcare services can be problematic for beneficiaries who live alone or in areas with limited public transportation, and this provision ensures that these individuals can still receive the regular care they need without financial strain.
Another key feature of Medicare Advantage plans is the provision for over-the-counter allowances. Depending on the plan, beneficiaries may be provided with a monthly or quarterly stipend to spend on over-the-counter items such as vitamins, cold medications, and other health-related goods. This benefit can substantially ease the financial burden for those who need regular over-the-counter supplies, aiding in preventive care measures.
One of the innovative offerings from certain Medicare Advantage plans is telehealth services, which have become increasingly important. With telehealth, beneficiaries can access healthcare professionals from the comfort of their home, an invaluable service that grew in importance during the COVID-19 pandemic. This service not only expands access to healthcare but also helps those with mobility restrictions or those living in rural areas maintain regular contact with healthcare providers without the need for travel.
The variety of benefits offered by Medicare Advantage plans underscores their appeal to a broad range of healthcare needs. From additional healthcare services to innovative health programs, these benefits collectively cater to specialized needs that traditional Medicare doesn’t address. Beneficiaries considering Medicare Advantage should evaluate these benefits closely to ensure they meet their health requirements, facilitating better healthcare engagement and outcomes. For personalized plan comparisons and more detailed information on specific benefits, beneficiaries can visit MedicarePartCPlans.org to make informed coverage choices.
Navigating Federal Regulations for Medicare Advantage
Understanding the complexities of federal regulations governing Medicare Advantage plans is crucial for beneficiaries seeking the right coverage. The Centers for Medicare & Medicaid Services (CMS) play a critical role in overseeing these managed care plans to ensure they meet specific standards and serve the diverse needs of enrollees. This section will delve into CMS’s regulatory responsibilities and highlight key federal regulations that impact advantage insurers. By grasping these regulatory frameworks, beneficiaries can navigate the Medicare Advantage landscape with greater confidence and clarity.
The Role of CMS in Regulating Medicare Advantage Plans
The Centers for Medicare & Medicaid Services, commonly known as CMS, is the federal agency tasked with the pivotal role of regulating Medicare Advantage plans. This branch of the federal government ensures that all participating insurers adhere to rigorous standards designed to protect the interests of enrollees. Catering to the dynamic needs of Medicare beneficiaries, CMS plays a vital role in maintaining the integrity and efficiency of the Medicare program.
By setting benchmarks and providing a comprehensive governing framework, CMS ensures that Medicare Advantage plans offer predictable and fair benefits, making healthcare more accessible and tailored to individual needs.
Medicare Advantage, also referred to as Medicare Part C, operates within the boundaries established by CMS regulations. These regulations govern areas such as plan design, benefits, payments, and risk adjustment methodologies. The risk adjustment process is particularly significant as it adjusts payments to health plans based on the health status and demographic profile of enrollees, thus ensuring that plans covering higher-risk individuals receive adequate compensation. This regulatory oversight is essential to prevent plans from solely targeting healthier individuals, thereby maintaining an equitable distribution of healthcare resources.
CMS also plays a vital role in the determination of accountability benchmarks for Medicare Advantage plans. These benchmarks influence the plans’ payment structures, ensuring that insurers receive appropriate compensation while maintaining affordability and quality of care for beneficiaries. Insurers are required to submit bids to CMS detailing how they intend to provide coverage to enrollees, which are then comparative analyzed against these benchmarks. This meticulous process ensures that Medicare Advantage plans align with federal standards, promoting fair pricing and comprehensive coverage.
Moreover, CMS issues clear guidelines to monitor the marketing practices of Medicare Advantage insurers. The federal government mandates transparency to prevent misleading marketing strategies that could potentially exploit enrollees or distort the perceived benefits of a plan. This regulatory framework aids beneficiaries in making informed choices by providing access to accurate and transparent information about their potential plans. CMS’s stringent rules on plan marketing ensure that beneficiaries receive truthful representations about coverage options, ultimately supporting better decision-making processes.
By regulating these many facets of the Medicare Advantage landscape, CMS ensures that advantage insurers operate with transparency, accountability, and a commitment to offering real benefits to enrollees. For beneficiaries, understanding CMS’s role reveals why their coverage options are structured the way they are, providing essential insight into the machinations of Medicare Advantage plans. Knowledge of these regulations can empower beneficiaries to leverage resources like MedicarePartCPlans.org, further bolstering their ability to select plans that align with their healthcare needs and preferences.
Key Federal Regulations Affecting Advantage Insurers
Federal regulations affecting Medicare Advantage insurers are comprehensive and multifaceted, designed to uphold the standards of the Medicare program while ensuring that advantage insurers provide enrollees with adequate, coverage. Notably, CMS’s oversight extends into several critical areas impacting how these plans operate and are structured, ensuring that they meet both the regulatory requirements and the expectations of beneficiaries.
One of the key regulations centers around the structure of benefits and payments. Medicare Advantage insurers must offer benefits that are comparable, if not superior, to those provided under traditional Medicare. This regulation ensures that advantage plans are not only competitive but also advantageous for beneficiaries who might require more than the basic Medicare benefits. This includes additional services like vision, dental, and hearing coverage not present in standard Medicare plans.
Furthermore, CMS regulates the cost-sharing aspects of Medicare Advantage plans, mandating that insurers offer plans with predictable out-of-pocket costs for enrollees. This is accomplished through regulations regarding copayments, deductibles, and coinsurance, which must be structured in a manner that does not overly burden beneficiaries financially. Insurers must also offer a variety of plans to accommodate different risk profiles and healthcare needs, contributing to a diverse marketplace where enrollees can find plans that best suit their financial and health circumstances.
Risk adjustment is another crucial regulatory component that directly impacts how insurers design their Medicare Advantage plans. This federal system ensures plans receive payments proportional to the risk levels of their enrollees, safeguarding against the potential neglect of higher-risk individuals who may require more extensive care. By instituting this risk adjustment framework, CMS ensures a balanced approach to care while preventing insurers from favoring only the healthiest populations, thus maintaining comprehensive inclusivity in plan offerings.
Compliance with CMS reporting requirements is another key regulative area for Medicare Advantage insurers. Insurers are required to report comprehensive plan details, including quality performance metrics, enrollees’ health outcomes, and plan safety issues. This ensures ongoing accountability and helps beneficiaries make educated decisions regarding their healthcare options. Through these requirements, CMS continuously monitors plan effectiveness and adherence to federal standards.
Another essential regulation concerns special enrollment periods. These allow eligible Medicare beneficiaries the opportunity to enroll in or switch Medicare Advantage plans outside of standard enrollment windows under specific circumstances, such as relocating or experiencing a significant change in their health status. Such federal regulations grant beneficiaries needed flexibility to adjust their healthcare coverage as their life situations change, ensuring they remain in plans that best meet their evolving health and financial needs.
Comprehending these federal regulations equips Medicare and those considering Medicare Advantage plans with the knowledge to make informed decisions. The layered regulatory environment crafted by CMS not only protects beneficiaries but also fosters a competitive and dynamic landscape where plan quality and accountability are prioritized. For those navigating these plans, resources such as MedicarePartCPlans.org provide valuable insights and tools for evaluating options based on geographic location and coverage needs.
Find & Compare Plans Online
Choosing the Right Medicare Advantage Plan
Deciding on the right Medicare Advantage plan can seem daunting, but having the right tools and information can make the process much easier. Medicare Advantage, also known as Medicare Part C, provides an alternative to traditional Medicare by offering comprehensive health plans through private insurers. It’s crucial to compare options based on your personal health needs, financial situation, and preferred coverage. Using location-based plan comparison tools and understanding plan costs and coverage options are essential steps in selecting a plan that offers the best health benefits for your specific circumstances.
Using Location-Based Plan Comparison Tools
Location-based plan comparison tools are indispensable for anyone exploring Medicare Advantage options. These tools assist beneficiaries by providing detailed information about the Medicare Advantage plans available based on their geographic area. Medicare Advantage plans differ by location, reflecting various factors such as local healthcare provider networks, plan popularity, and regional healthcare needs. Thus, utilizing a plan comparison tool that takes location into account helps ensure that beneficiaries find the most suitable plans tailored to their local environment.
Many of these tools are available online and are easily accessible. They allow users to input their zip code or city to view a variety of Medicare Advantage plans within their specific area. These tools compare health plans by assessing plan premiums, benefits, coverage levels, and network restrictions. They provide insights not only into the cost but also the quality of coverage offered, assisting beneficiaries in making informed decisions. It’s important to consider that different regions may offer different plan options and pricing structures due to varying competition among insurers.
Platform tools like the one available on MedicarePartCPlans.org are designed to be user-friendly, enabling beneficiaries to compare plans quickly and efficiently. These resources offer a wealth of information that can be personalized according to health needs, budget considerations, and preferred health care services. Beneficiaries should evaluate Medicare Advantage plans based on comprehensive coverage that includes additional benefits such as dental, vision, and prescription drug services that may vary by location.
Furthermore, these tools often contain valuable user reviews and ratings, which provide additional consumer insights. While comparing Medicare Advantage plans, it’s helpful to read reviews from current enrollees who have firsthand experience with the plan’s customer service, network quality, and overall satisfaction. By leveraging both feature comparison and peer insights, beneficiaries can form a well-rounded view of how a particular plan might fit their needs.
When considering whether a specific Medicare Advantage plan is right for you, ensure that the chosen plan’s provider network includes your preferred doctors and medical facilities. Some plans may have network restrictions, which can limit your ability to receive services from providers outside the plan’s network. Verifying in-network providers helps avoid unexpected costs and ensures continuity of care. Medicare Advantage plans, therefore, offer a personalized approach to health insurance, and using reliable, location-based plan comparison tools is a practical step towards finding a plan that aligns with individual health goals and geography.
Understanding Plan Costs and Coverage Options
Understanding the array of plan costs and coverage options is central to selecting a Medicare Advantage plan that aligns with your budget and health care needs. Medicare Advantage plans can vary widely in terms of premium costs, out-of-pocket expenses, and the range of services covered. As these are private insurance plans approved by Medicare, they offer benefits beyond those of traditional Medicare, often incorporating additional coverage like vision and dental, which can be enticing for many beneficiaries.
One of the first considerations when evaluating Medicare Advantage plans is the premium costs. Some beneficiaries might find plans with lower premiums, but should consider the trade-offs. Lower premiums can sometimes accompany higher out-of-pocket costs, such as copayments and deductibles. Therefore, it’s imperative to examine the total likely expenditure, considering both premiums and potential copayments for routine services, visits to specialists, or hospital stays. Beneficiaries should also look into whether the plan includes annual out-of-pocket maximums, which can shield them from excessive spending on health services within a given year.
Coverage options are equally essential when choosing between different Medicare Advantage plans. Each plan provides a different level of coverage, and reviewing the specific benefits is crucial. Beneficiaries should ensure that their primary care providers, specialists, and preferred hospitals are within the plan’s network. Also, check if the plan offers coverage for routine care and any additional services required for personal health needs. For instance, many Medicare Advantage plans offer wellness programs, chronic disease management, and sometimes alternative medicine options like acupuncture.
Another factor to consider is the inclusion of Part D, the prescription drug coverage, within the selected Medicare Advantage plan. Medication costs can constitute a substantial portion of healthcare expenses, particularly for those on long-term prescriptions. Integrating drug coverage within a Medicare Advantage plan simplifies management and often reduces total drug costs compared to purchasing a separate Part D plan. Beneficiaries should review formularies provided by plans to ensure that their required medications are covered and identify any restrictions or prior authorizations that could affect access.
Finally, beneficiaries may have different health care utilization patterns, influencing their ideal plan selection. For instance, those with chronic conditions may benefit from plans offering more generous coverage for specialist visits and frequent prescription refills. Conversely, beneficiaries who rarely access healthcare services might prefer plans with lower monthly premiums. Understanding one’s health history and anticipated needs is key to weighing different plan costs and coverage options effectively.
By carefully examining these factors, beneficiaries can avoid unexpected costs and ensure consistent access to necessary services. For more nuanced information and detailed plan comparisons, MedicarePartCPlans.org provides educational resources and a free plan finder tool to help identify Medicare Advantage plans that meet personal healthcare requirements effectively. Thus, understanding the dynamics of plan costs and coverage options enables beneficiaries to make informed decisions, ensuring comprehensive care while managing financial outlay.
| Key Considerations | Location-Based Plan Tools | Plan Costs & Coverage | Additional Benefits |
|---|---|---|---|
| Understand personal health needs and preferences | Utilize online tools for regional plan availability and user satisfaction | Review plan premiums and network restrictions | Check for supplemental services like dental and vision care |
| Consider the importance of plan flexibility | Access comparison tools for geographically tailored options | Evaluate potential out-of-pocket expenses | Explore the inclusion of prescription drug coverage |
| Assess potential changes in health status | Read user reviews to gauge plan performance in your area | Look for plans with preferred provider access | Determine the availability of wellness programs and services |
| Weigh the need for specialist access and services | Benefit from tools providing insights on best-rated plans near you | Account for deductibles and co-payment plans | Consider options for worldwide emergency coverage |
This table provides a compact overview of the essential aspects to consider when selecting a Medicare Advantage plan, including the tools and coverage options tailored to individual needs and locations.
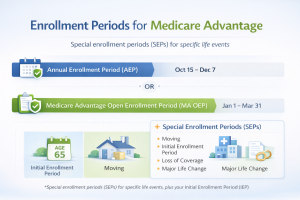
Enrollment Periods for Medicare Advantage
Choosing the right time to enroll in a Medicare Advantage plan is crucial to avoid penalties and ensure seamless coverage. Enrollment periods for these plans are regulated by the Centers for Medicare & Medicaid Services (CMS), providing specific windows during which beneficiaries can join, switch, or drop a plan. Understanding these periods helps you plan your healthcare wisely. This section covers everything from the initial enrollment period with its critical deadlines to the special enrollment periods designed to accommodate life changes that might affect your healthcare needs.
Initial Enrollment and Key Deadlines
Understanding the Initial Enrollment Period (IEP) is critical for new Medicare beneficiaries considering Medicare Advantage plans. This period is the first opportunity for eligible individuals to enroll in a Medicare Advantage plan and is closely regulated under federal guidelines. The IEP begins three months before you turn 65 and extends three months after, totaling a seven-month window during which you can choose a suitable plan that meets your healthcare needs.
During the IEP, beneficiaries have the flexibility to explore various Medicare Advantage plans without facing penalties or lapses in coverage. At this stage, evaluating plans based on your health conditions, preferred healthcare providers, and financial situation is paramount. Since Medicare Advantage plans are offered by private insurance organizations, they may vary significantly in coverage options and costs, making it vital to compare plans thoroughly. Key deadlines within this period can influence your initial plan selection, ensuring your healthcare aligns with both current and future needs.
For individuals already receiving Social Security or Railroad Retirement Board benefits before age 65, enrollment in Medicare is automatic, but enrolling in a Medicare Advantage plan requires proactive steps. This automatic process simplifies initial Medicare entry, but for a comprehensive health approach, considering Medicare Advantage’s additional benefits such as prescription drug coverage is advantageous. Evaluating whether these plans include benefits like dental, vision, or hearing can play a huge role in your overall coverage decision.
An important aspect during the IEP is the availability of additional assistance programs for those who might qualify based on income and resources. Programs like Medicaid and the Medicare Savings Program can ease the financial burden by assisting with premiums, deductibles, and other out-of-pocket costs. If eligible, these programs can be a lifeline, facilitating access to Medicare Advantage plans without substantial financial strain. It is essential to meet deadlines for applying to these programs, as late applications may delay benefits.
The IEP isn’t just a one-time window; it marks the starting point for your Medicare journey, setting the stage for decision-making about healthcare as your needs evolve. Missing the initial deadlines can lead to a Special Enrollment Period, often with conditions or penalties. Therefore, entering Medicare with a clear understanding of these key deadlines and preparation can prevent unexpected healthcare expenses and assure continuous, comprehensive coverage. For further guidance on plan costs and location-specific options, tools available on MedicarePartCPlans.org can aid in navigating this essential phase effectively.
Continue your understanding of the Initial Enrollment Period with these important considerations for choosing a Medicare Advantage plan:
- Review plan benefits to ensure they match your current and anticipated healthcare needs.
- Verify if your preferred healthcare providers are within the plan’s network.
- Evaluate plan costs, including premiums, deductibles, and copayments, that fit your financial situation.
- Consider additional benefits like dental, vision, or hearing that may be important to you.
- Investigate if the plan offers prescription drug coverage crucial for your medication needs.
- Explore eligibility for assistance programs that can offset Medicare-related expenses.
- Check location-specific plan availability to ensure access to providers near you.
Making informed choices during your IEP can shape your healthcare experiences positively for years to come.
Special Enrollment Periods and Eligibility Criteria
Life doesn’t always fit neatly within scheduled enrollment periods, and this is where Special Enrollment Periods (SEPs) offer vital flexibility for Medicare beneficiaries. These periods are designed to accommodate changes in your life circumstances that affect your healthcare coverage, allowing you to switch or enroll in a Medicare Advantage plan outside the standard periods without facing penalties. Understanding SEPs can ensure your healthcare needs are continually met, even as your circumstances change.
Several triggering events qualify you for a SEP. Moving to a new location outside your current plan’s service area, losing other health coverage, or significant changes in your financial situation, such as the loss of Medicaid eligibility, are common qualifiers. These events permit you to adjust your Medicare Advantage plan to better suit your new circumstances, ensuring continuous access to health services without disruption.
Eligibility criteria for SEPs vary, often mandated by specific timing and documentation requirements. For instance, if you relocate, you typically have two months from your move date or the date your current plan’s service area no longer covers you to select a new Medicare Advantage plan. Prompt action is essential to avoid lapses in coverage, particularly if your health conditions require regular medical attention. Similarly, if enrolling due to loss of coverage, you’ll need to provide proof of your previous coverage’s termination.
For beneficiaries experiencing changes in financial status, SEPs provide crucial relief especially if you become eligible for assistance programs like Medicaid or Extra Help. These programs help cover the costs of medication or monthly premiums, ensuring your healthcare costs remain manageable. Adjustments during a SEP allow beneficiaries to switch to a Medicare Advantage plan that integrates these programs, minimizing out-of-pocket expenses.
Understanding these periods requires a thorough examination of your current health status and future healthcare needs. Evaluating the regional availability of health plans using resources like MedicarePartCPlans.org can help identify providers and benefits that align with your circumstances, whether new or changing. SEPs provide peace of mind by ensuring your healthcare is as dynamic as your life itself, offering opportunities to optimize your plan as circumstances require.
Ultimately, Special Enrollment Periods exist to ensure Medicare Advantage plan holders experience uninterrupted care irrespective of life’s uncertainties. They enable beneficiaries to address evolving healthcare needs, support continuous coverage adaptation, and leverage location-specific benefits, helping maintain healthcare fulfillment even amidst change. Utilize tools on MedicarePartCPlans.org not only to understand available SEPs in your region but also for seamless plan comparison and selection tailored to updated personal health and financial circumstances.
Understanding the regulations and oversight provided by CMS on Medicare Advantage plans is crucial for making informed decisions about healthcare coverage. By staying informed about how these plans operate under federal statutes, you can better navigate the options available to suit your individual needs. MedicarePartCPlans.org is here to assist in demystifying these regulations, offering clarity on what to expect, and helping compare plans based on location and coverage needs. With comprehensive resources and educational tools, we aim to empower beneficiaries to make confident, well-informed choices regarding their healthcare options.
Compare plans and enroll online
Frequently Asked Questions
What is Medicare Advantage and how is it regulated?
Medicare Advantage, also known as Medicare Part C, offers an alternative to traditional Medicare by providing coverage through private insurers. These plans are regulated by the Centers for Medicare & Medicaid Services (CMS) to ensure they meet federal standards and provide comprehensive benefits.
How do Medicare Advantage plans differ from traditional Medicare?
Medicare Advantage plans differ from traditional Medicare by bundling coverage for Parts A, B, and often Part D, into one plan offered by private insurers. These plans often include additional benefits such as dental, vision, and prescription drug coverage which traditional Medicare does not typically offer.
What additional services do Medicare Advantage plans offer?
Medicare Advantage plans may provide additional benefits like dental, vision, hearing, wellness programs, and sometimes fitness memberships. They also might offer telehealth services, transportation for medical appointments, and over-the-counter allowances.
What are Special Enrollment Periods (SEPs) in Medicare Advantage?
Special Enrollment Periods (SEPs) allow beneficiaries to enroll in or modify their Medicare Advantage plans outside of standard enrollment times due to life changes such as moving or losing other health coverage. SEPs provide flexibility without penalties.
How can Medicare beneficiaries use location-based comparison tools effectively?
Location-based comparison tools help beneficiaries compare Medicare Advantage plans in their area. By entering their zip code, they can view plans available locally, assess premiums and coverage levels, and find plans tailored to regional healthcare needs.
Have Questions?
Speak with a licensed insurance agent
1-877-436-2343
TTY users 711
Mon-Fri: 8am-9pm ET
Find & Compare Plans Online
ZRN Health & Financial Services, LLC, a Texas limited liability company

