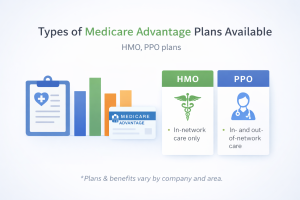
Navigating Medicare Advantage Plans in New York can feel overwhelming, especially with multiple options and ever-changing regulations.
As a trusted Medicare insurance broker with 15 years of expertise, we help New York residents find plans that best fit their healthcare and budget needs.
Whether you are evaluating your options for the first time or seeking better benefits, understanding how Medicare Advantage plans work in New York empowers you to make an informed choice.
Plan availability, costs, and provider networks can vary widely based on county and service area. What works well in one part of the state may not be available in another, which makes local knowledge especially important.
Medicare Advantage plans may include additional services, structured networks, and annual cost limits that appeal to many beneficiaries.
Learning how coverage options differ by location, benefit structure, and provider access helps New York residents compare plans with confidence and choose coverage that aligns with their medical needs and financial goals.