Enrolling in Medicare Part C, also known as Medicare Advantage, is a vital step for those looking to expand their healthcare coverage beyond Original Medicare. This webpage will help you navigate the process, understand what Part C covers, including hospital and medical services, and guide how to enroll. With options varying by location, it’s essential to explore the available plans and find one that aligns with your healthcare needs and budget. Utilize our free tool to compare plans, ensuring you have access to comprehensive benefits and the medical care you require.





Enrolling in Medicare Part C
Key Highlights
- Medicare Part C combines Parts A and B with additional benefits like vision and dental.
- Advantage plans may have networks but often offer lower cost-sharing than Original Medicare.
- Eligibility requires enrollment in Medicare Parts A and B, and residence in the plan’s service area.
- Enrollment periods include the Initial Enrollment, Annual Enrollment, and Open Enrollment Periods.
- Use the Medicare plans finder tool to compare options and tailor your healthcare coverage.
Compare plans and enroll online
Understanding Medicare Part C: Coverage and Benefits
Medicare Part C, commonly known as Medicare Advantage, offers beneficiaries an alternative to Original Medicare by providing comprehensive healthcare coverage through private insurance plans. These plans include all the benefits of Parts A and B and often provide additional benefits like vision, dental, and prescription drug coverage. By choosing a Medicare Advantage plan, beneficiaries can enjoy more expansive coverage options tailored to their specific healthcare needs. This section delves into what a Medicare Part C plan offers and how these plans differ from Original Medicare, helping you to understand which healthcare coverage suits your needs best.
| Feature | Original Medicare | Medicare Advantage |
|---|---|---|
| Coverage | Part A (Hospital) and Part B (Medical) | Includes Part A and B, often with additional benefits |
| Prescription Drugs | Requires a separate Part D plan | Often included in the plan |
| Benefits | Standardized offerings | May offer vision, dental, and hearing services |
| Cost Structure | Medicare Part A is free for most; Part B has a premium | Varies by plan; may include lower out-of-pocket costs |
| Network Flexibility | No network restrictions; see any provider that accepts Medicare | Typically requires using the plan’s network of providers |
This table outlines the distinctions between Original Medicare and Medicare Advantage plans, summarizing key features to aid in informed decision-making regarding healthcare coverage options.

What a Medicare Part C Plan Offers
Medicare Part C, also referred to as a Medicare Advantage plan, combines coverage from both Medicare Part A (hospital insurance) and Medicare Part B (medical insurance), often with additional benefits not available through Original Medicare. When you opt for Part C, you’re usually receiving healthcare coverage from private companies that Medicare approves, offering more localized options that can cater to your specific healthcare needs. These plans typically include additional benefits like vision, dental, and hearing services, which are not covered under Original Medicare. Moreover, many Medicare Advantage plans offer prescription drug coverage, consolidating healthcare services into a single, comprehensive plan.
Another notable feature of Medicare Advantage plans is their cap on out-of-pocket expenses. Original Medicare does not limit the amount you might spend out-of-pocket, but Medicare Part C plans set a maximum that provides beneficiaries with greater financial predictability and protection. Furthermore, Medicare Advantage plans often include a network of preferred healthcare providers and facilities. While these networks can sometimes restrict where you receive covered services, they often translate to lower cost-sharing for covered participants, making healthcare more affordable. However, it’s crucial to review each plan’s specific network and drug formulary to ensure preferred physicians and prescriptions are included.
For those who need specialized care or manage chronic conditions, certain Medicare Advantage plans, often called Special Needs Plans (SNPs), tailor coverage to meet those needs. These plans focus on offering specialized treatments and medication management, which can be particularly beneficial for individuals dealing with chronic health conditions. Given these varied plan options, using a comparison tool, such as the one offered on MedicarePartCPlans.org, can help beneficiaries explore the differences and select a plan that aligns with their healthcare coverage needs and budget.
To further explore the diverse offerings and features of Medicare Part C plans, consider these key aspects:
- Ensure vision and dental benefits align with your healthcare priorities.
- Compare plans for comprehensive prescription drug coverage.
- Review network restrictions related to preferred healthcare providers.
- Evaluate out-of-pocket expense caps for financial predictability.
- Understand the benefits of Special Needs Plans for chronic conditions.
- Investigate prescription formularies for necessary medications.
- Use comparison tools to tailor-plan choices to your needs.
Understanding these elements can aid in making informed decisions about Medicare Part C plans.

How Medicare Advantage Plans Differ from Original Medicare
Choosing between a Medicare Advantage plan and Original Medicare requires an understanding of their key differences in coverage, benefits, and flexibility. Original Medicare, comprised of Part A and Part B, provides standardized benefits, offering uniform hospital and medical insurance coverage to all beneficiaries. Yet, Original Medicare often leaves significant gaps in coverage, such as prescription drugs, dental, and vision care, requiring individuals to seek additional plans like Medigap for comprehensive coverage.
In contrast, Medicare Advantage plans cover everything Original Medicare offers but often bundle additional healthcare services into a single plan, potentially simplifying management and delivering a more holistic approach to health care. These plans differ significantly as they operate like health maintenance organizations (HMOs) or preferred provider organizations (PPOs), which usually means beneficiaries need to follow more structured healthcare networks for their care needs. This can mean less flexibility in choosing providers, but often translates to lower costs and more predictable spending limits.
The cost of Medicare Advantage plans can also vary depending on the plan specifics and location, which might be an attractive feature for those seeking affordable healthcare coverage. They can have low or even $0 premiums, though they often come with copayments and coinsurance. It’s essential to weigh these costs against the benefits and the flexibility each plan offers, ensuring it aligns with your healthcare priorities. Medicare Advantage plans may include wellness programs and additional benefits like gym memberships, adding another layer of value not covered by Original Medicare.
This divergence in structure and additional benefits allows Medicare Advantage plans to cater to specific groups needing more than Original Medicare provides. The choice between these options should be guided by evaluating what matters most for your individual healthcare needs and financial situation. For more clarity on making the right decision for your circumstances, using resources such as MedicarePartCPlans.org can provide guidance in comparing coverage options tailored to your needs and location.
Eligibility Requirements for a Medicare Advantage Plan
Understanding the eligibility requirements for enrolling in a Medicare Advantage plan is crucial for beneficiaries seeking comprehensive healthcare coverage. Medicare Advantage, also known as Part C, combines the health benefits of Parts A and B, frequently offering additional perks like vision and dental services. Navigating through the enrollment processes involves knowing who qualifies, recognizing any restrictions or qualifications that might influence availability, and aligning options with healthcare needs. This section sheds light on who can enroll in a Part C plan and what restrictions or qualifications might apply, ensuring you’re well-equipped to make informed decisions about your healthcare options.
Find & Compare Plans Online
Who Can Enroll in a Part C Plan
Medicare Advantage plans, or Part C, are designed to offer a blend of comprehensive healthcare services that often attract those looking to maximize their healthcare benefits. To enroll in a Part C plan, you must first meet the basic eligibility requirements set by Medicare. Primarily, you need to be enrolled in both Medicare Part A (hospital insurance) and Medicare Part B (medical insurance). This is crucial as Medicare Advantage plans build upon the foundation provided by these parts, integrating benefits from both to cover a wider range of healthcare needs.
In addition to being enrolled in parts A and B, those wishing to join a Medicare Part C plan should reside within the plan’s service area. This requirement ensures beneficiaries have access to participating providers and facilities within their locale, an important feature since many Advantage plans operate like health maintenance organizations (HMOs) or preferred provider organizations (PPOs). These structures can offer significant cost savings but often necessitate using specific networks, so ensuring your residence aligns with an available plan’s service area is key.
Moreover, anyone wishing to enroll in a Medicare Advantage plan must not suffer from end-stage renal disease (ESRD), although recent changes have allowed more individuals with specific health conditions to be eligible under certain plan types, such as those designed for beneficiaries with chronic illnesses. Ensuring you meet these basic Medicare eligibility criteria is your first step toward enrolling in a Part C plan. Also, reviewing different plan types and benefits through resources and tools, like our plan finder on MedicarePartCPlans.org, can help streamline the decision-making process and assist in finding a plan tailored to your health care priorities.
Understanding Any Restrictions or Qualifications
While Medicare Part C offers enhanced healthcare benefits compared to Original Medicare, understanding the restrictions or qualifications associated with these plans is crucial for seamless healthcare management. An important qualification involves your timing during the Medicare enrollment periods. Typically, Medicare Advantage plans can be joined during the Initial Enrollment Period when you first become eligible for Medicare, or during the Annual Enrollment Period occurring every fall. Missing these periods can mean waiting until the next window, potentially delaying benefits.
Certain restrictions also apply regarding plan specifics and healthcare providers. Many Medicare Advantage plans operate within network settings, HMO or PPO, which might limit the choice of doctors or hospitals compared to Original Medicare. These networks aim to control healthcare costs and enhance service coordination, but enrollees must consider whether preferred providers comply with their chosen plan. Additionally, plans may change annually, with new providers added or removed, so staying informed about network changes is essential.
It’s also beneficial to understand the coverage limits and costs associated with Part C plans. Coverage may include extras like vision, dental, and hearing services, not typically covered by Original Medicare. However, while additional benefits address broader healthcare needs, each plan sets specific coverage boundaries and out-of-pocket maximums you should be aware of. Plans also differ regionally, influencing availability and coverage scope, emphasizing the importance of reviewing plan offerings based on your location.
For those managing chronic conditions, considering a Special Needs Plan (SNP) that caters specifically to your healthcare scenario might be advantageous. Resources offered by MedicarePartCPlans.org provide comparative tools to evaluate these plans and comprehend all related restrictions efficiently. Being proactive in understanding these plan qualifications expedites enrollment and ensures continuous access to proper healthcare services tailored to your circumstances.
The Medicare Enrollment Process: Timing and Steps
Navigating the Medicare enrollment process can seem daunting, but understanding the right timing and steps can simplify your journey. As you consider enrolling in Medicare Advantage, also known as Part C, it’s essential to recognize key enrollment periods and how they align with your healthcare goals. This overview will delve into the various enrollment periods, highlight the necessary steps for enrolling in an Advantage plan, and explain how these plans build upon the foundation of Original Medicare, Parts A and B, to offer comprehensive coverage with potential additional benefits.
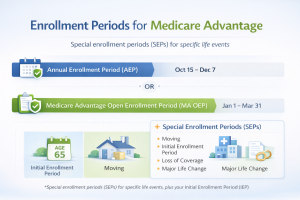
Key Medicare Enrollment Periods to Consider
Understanding the Medicare enrollment periods is crucial as you contemplate enrolling in a Medicare Advantage plan. The initial pathways into Medicare typically open during what is known as the Initial Enrollment Period (IEP). This seven-month period begins three months before you turn 65, includes your birthday month, and continues for three months afterward. During this time, you can enroll in Original Medicare, which is a prerequisite for selecting an Advantage plan. Enrolling during the IEP helps ensure your coverage begins as soon as you’re eligible.
Beyond the IEP, the Annual Enrollment Period (AEP) is another significant window for Medicare enrollees. Occurring from October 15 to December 7 each year, the AEP allows beneficiaries to switch from Original Medicare to a Medicare Advantage plan, change Advantage plans, or even elect a different prescription drug plan. This period is vital for those wishing to reassess their healthcare needs and make adjustments to their plans to align with changes in personal health conditions or financial priorities. Missing this timeframe means waiting until the next AEP to make any changes.
The Medicare Advantage Open Enrollment Period (OEP), from January 1 to March 31, offers a further opportunity for beneficiaries already enrolled in a Medicare Advantage plan to switch to another Advantage plan or return to Original Medicare. This additional period provides a second chance to optimize your healthcare coverage for the year. It should be noted, however, that during the OEP, you can’t switch from Original Medicare to a Medicare Advantage plan. Having an understanding of these enrollment periods is integral to maximizing your coverage options. At MedicarePartCPlans.org, our free Medicare plans finder tool can be instrumental in aligning the right Advantage plan with your healthcare objectives efficiently and effectively.
Navigating the enrollment process for Medicare Part C can be simplified by understanding both the coverage benefits and enrollment steps. By evaluating your healthcare needs and comparing available plans tailored to your location, you can make an informed decision about your Medicare coverage. For further assistance, consider using tools like the Medicare plans finder, which can help match you with options that meet your specific health and budgetary requirements. Always keep track of enrollment periods to ensure you secure the Medicare Part C benefits aligned with your personal health care goals.
Compare plans and enroll online
Frequently Asked Questions
What is Medicare Part C?
Medicare Part C, also known as Medicare Advantage, is an alternative to Original Medicare. It is offered through private insurance companies and combines Part A (hospital insurance) and Part B (medical insurance), often including additional benefits like vision, dental, and prescription drugs.
What are the enrollment periods for Medicare Advantage?
Enrollment periods for Medicare Advantage include:
- Initial Enrollment Period (IEP): Starts three months before you turn 65, includes your birthday month, and ends three months after.
- Annual Enrollment Period (AEP): October 15 to December 7, allowing changes in Medicare plans.
- Medicare Advantage Open Enrollment Period (OEP): January 1 to March 31, allowing changes within Medicare Advantage plans.
Utilizing these periods ensures you can manage your Medicare Advantage plan effectively.
What makes Medicare Advantage plans different from Original Medicare?
Medicare Advantage plans cover all the benefits of Original Medicare and often include additional services like vision, dental, and hearing. They typically operate within a network of providers and have a cap on out-of-pocket expenses, offering financial predictability.
Who is eligible for Medicare Part C?
To be eligible for Medicare Part C, you must be enrolled in both Medicare Part A and Part B, and reside in the plan’s service area. Some individuals with specific health conditions may also be eligible under Special Needs Plans (SNPs).
How can I compare different Medicare Advantage plans?
You can use tools like the Medicare plans finder on MedicarePartCPlans.org to explore and compare different Medicare Advantage plans. This allows you to evaluate how each plan aligns with your specific healthcare needs and budget.
Have Questions?
Speak with a licensed insurance agent
1-877-436-2343
TTY users 711
Mon-Fri: 8am-9pm ET
Find & Compare Plans Online
ZRN Health & Financial Services, LLC, a Texas limited liability company

